Food is very powerful information. When choosing which foods to eat, it is vital to understand how food talks to your cells. Certain types of food increase the amount of systemic inflammation in your body, while other foods modulate your immune system towards a healthy inflammatory response. Knowing the “why” of your food helps to better understand “what” foods to choose. Move beyond will-power to insight.
Mechanism: The gut-immune connection
One very important food-immune interface happens in your gut. Your upper gut works to digest and assimilate food including macronutrients like carbohydrates, protein, and fat as well as minerals and vitamins such as B12, iron, zinc, vitamin C and vitamin D. There are undigested fibers (prebiotics) that go on to “feed” the trillions of bacteria that live in the large intestine called the “gut microbiome.”
Current research continues to exhibit how this microbial ecosystem complexly interacts with the immune system to affect systemic responses. When this system works optimally, the gastrointestinal tract sends appropriate signals of safety or danger to the immune system which affects the level of systemic tolerance or reactivity.

Key principles for optimizing the gut-immune connection
- Enhancing upper gut digestion and absorption (stomach and small intestine)
You can make the healthiest meal, but if your gut does not break it down correctly or absorb it, your cells will not see those nutrients. Cells that do not get the key nutrients for critical cell functions send error signals that the immune system then interprets as danger signals which can provoke an acute or chronic inflammatory response.
- Supporting microbiome diversity
Turns out you aren’t just eating for yourself. To optimize the gut-immune connection, you want to think of what your microbiome likes to eat. Prebiotics are dietary fibers that feed the “friendly” bacteria in your gut to improve both local gut function and systemic immune function.
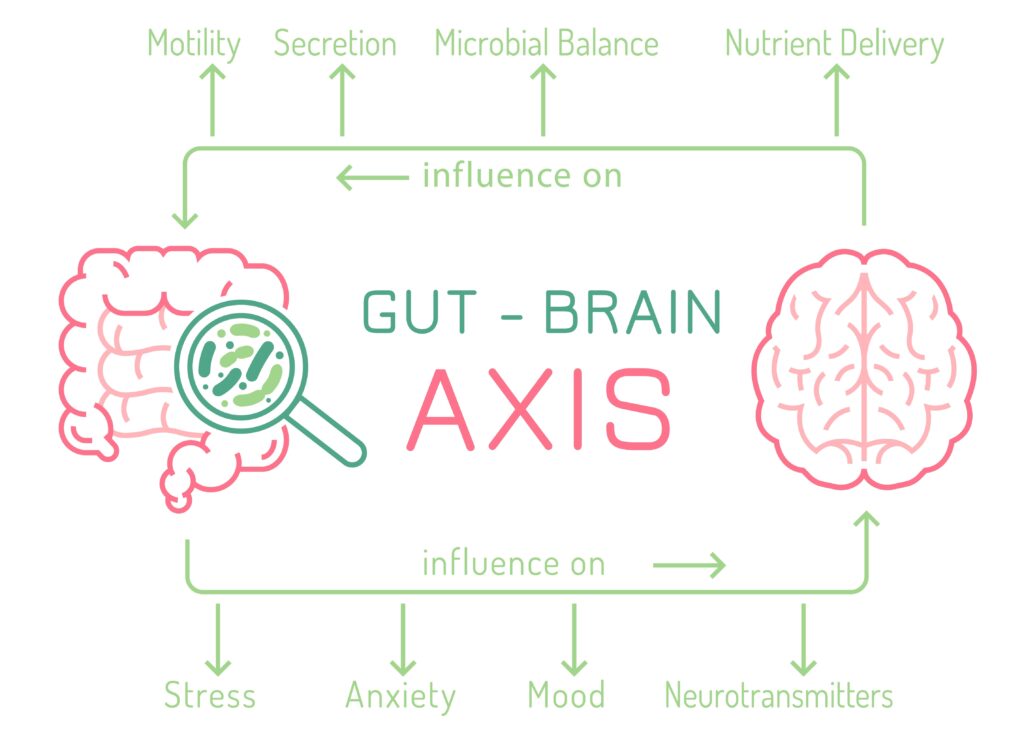
- Utilizing the brain and gut axes
The brain and gut operate on a bi-directional axis. Information from the gut impacts function in the brain. Information from the brain impacts the function of the gut including how the gut digests, produces protective mucus, and how food moves through the intestines.
Now let’s look at a couple of examples to put these principles into action.
Meal #1:
Squeezing a quick meal on the go after work. Pulling through the fast-food takeout window with a super-sized value meal with french fries, chicken tenders, and a large soda. Eating quickly, while sitting in traffic listening to an exasperating news report on the radio.
- Effects of distracted and fast eating on upper gut function
The upper gut is cued by the brain during the anticipatory phase of eating to initiate the release of stomach acid and digestive enzymes. In this example, eating in a distracted state (i.e. while driving, listening to the radio, rushing on the go) alters the initiation of digestive cues which can lead to maldigestion.
Effects of this include bloating, gas, acid reflux, belching, abdominal pain, and loose stools. In addition, incorrectly digested proteins and fats have a negative impact on the microbiome and can increase systemic inflammation.
- Processed food and impacts to the microbiome
Ultra-processed foods found in this meal are calorically dense (i.e. sugar, salt, fat) and stripped of fiber. This is a bad combination. Your gut absorbs the macronutrients such as carbohydrates and fat efficiently and quickly which has negative impacts to your metabolic function (i.e.: blood sugar and cholesterol).
In addition, there is no good fiber in this meal to feed your microbiome. These combinations of factors have been shown in studies to increase inflammatory markers in the bloodstream for multiple hours after ingestion of this type of meal.
- Eating in a stressed state
Our emotional state affects the signals our brain sends to our gut. Even though the nutrient quality of this meal could be much better, eating in an emotionally reactive state such as anger or fear creates a different brain-gut signal which has been shown to create greater “danger signals” to your immune system from your brain and gut.

Meal #2:
Sitting down as a family for Sunday dinner. Starting the meal with a prayer of gratitude before sharing herb crusted salmon, sauteed Hamakua mushrooms with ghee, broccoli with garlic, and multi-color cabbage coleslaw. Eating slowly while enjoying conversation.
- Effects of eating slow on upper gut function
Stretch receptors in the stomach are activated as it fills with food or water. Eating slowly allows the brain and gut to work in better synchrony with bi-directional signaling to reduce over-eating.
Excessive caloric intake has been shown to increase inflammation in fat cells and release fatty acids into other tissues including liver and muscle cells. Eating slowly and consciously allows us to be more present to our body’s cues of fullness to reduce over-consumption of calories.
- Variety of plant fibers: “eating the rainbow”
You don’t have to be a dietician to create a plate designed to make your microbiome happy. Consuming a variety of colors of vegetables across different families (such as herbs, mushrooms, broccoli, cabbage, garlic in the example meal) break down into a feast for your microbiome.
Ghee is full of butyrate which is also a superfood for the gut. When you feed your microbiome with these wonderful foods, your microbiome will pay you back with important safety signals to your immune system.
- Impacts of gratitude on gut and immune function
The act of eating in community, sharing a meal with gratitude, and the feeling of support has been shown to improve immune function. Nourishment from a meal isn’t just in the food you are eating.
The company and environmental cues influence signals to your brain that can have profound effects on how your body digests and assimilates food as well as directly on your immune system itself.
Ultimately, we want to create the conditions for your body to produce a healthy inflammatory response. An optimal immune system is one that readily defends, protects, and repairs. This regulatory “checks and balances” is key to your optimal health.
If you are struggling with a dysregulated immune response, we look forward to helping you create a dietary and lifestyle strategy to optimize your gut-immune function towards greater tissue healing and function.